Orofacial Myofunctional Therapy
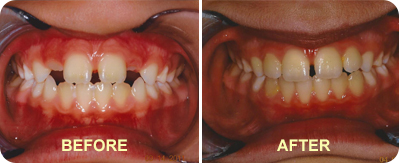
View our Myofunctional Therapy Before & After Photos!
Check out our album full of case studies for Mouth Breathing, Sucking Habits, and Tongue Thrust
We are SD Regional Center vendors and offer FREE speech therapy, occupational therapy, and physical therapy services for those children that qualify! Our physical therapy team is also in-network with nearly all insurance companies!
We Work With Patients Of All Ages To Help Treat The Following Issues:

- Thumb, Finger, Pacifier, and Other Negative Oral Habits
- Mouth Breathing and Open Lips/Mouth Posture
- Tongue Thrust for Speech and Speech Articulation Issues
- Tongue Thrust for Chewing and Swallowing
- Incorrect Tongue Positioning at Rest
- Drooling
- Chewing and Eating Difficulties
- Sleep-Related Breathing Issues (including snoring and sleep apnea)
- Bruxism (Clenching and Grinding)
- TMJ Dysfunction
- Mouth, Face, and Jaw Muscle Problems and Pain
- Orthodontic cases (including orthodontic relapse)
- Our Speech-Language Pathologists team up with our Doctors of Physical Therapy to help treat co-occuring postural problems, forward head posture, neck pain and tension, facial pain and tension, headaches, migraines, vertigo, balance issues, and breathing dysfunction utilizing specialized and advanced Postural Restoration Institute (PRI) techniques
We work with many orthodontists resolving the myofunctional issues of patients in order to help the teeth and mouth achieve a desired position pre, during, and post orthodontics. Myofunctional therapy can also help prevent orthodontic relapse once orthodontic appliances are removed.
What Sets Us Apart
In 2015, we were chosen to partner with and then take over the practice of the distinguished Katha Phair, Certified Orofacial Myologist, who is nationally renowned for her 40 years of dedication to successfully treating thousands of myofunctional patients and advancing the entire field of myofunctional therapy. Katha Phair has been recognized as an authority in the field of orofacial myology, and our myofunctional therapists trained intensely with Katha in her advanced and specialized evaluation and treatment techniques. We are the only therapists that have ever received this specialized training. Because of our reputation and the amazing progress that our patients make, we receive referrals from over 150 dentists, orthodontists, and medical specialists. Our myofunctional therapists are constantly advancing their education in the field and working to educate other professionals and patients about the benefit of our services. We are dedicated to working as a team with your dentist, orthodontist, ENT, or other specialist to make sure you receive the best care. Based on our advanced training and techniques, we are dedicated to treating our patients with the highest level of expertise. The before and after pictures and speak for themselves! We are more than delighted to offer this specialized service and to watch the positive results our patients make.
What also sets us apart is our holistic, team approach to the assessment and treatment of orofacial myofunctional disorders. We are one of the only offices in the country that has teamed up with physical therapists who are also trained in myofunctional therapy to treat our patients with co-occuring issues including issues with posture, headaches, head/face/neck tension, pre- & post- tongue tie release, TMJ problems, dysfunctional breathing patterns, vertigo, balance issues, and muscle tone problems, to name a few. We are able to assess and treat patients as a team. This allows for more thorough and comprehensive treatments for patients of all ages.
WHAT IS MYOFUNCTIONAL THERAPY?
- Physiologic Rest Posture
- Saliva swallowing
- Chewing and swallowing food
- Liquid swallows
- Speech
Myofunctional Therapy correctS the improper function of the tongue and facial muscles for the mouth functions. A proper physiologic rest posture of the mouth includes the following:
- The tongue should be positioned on the roof of the mouth behind the upper teeth.
- The jaws should be slightly apart.
- The lips should be closed.
- Breathing should be through the nose.
In a tongue thrust, the tongue pushes against or between the front or side teeth during chewing, swallowing, and/or speaking, rather than lifting up to the roof of the mouth. When the mouth does not rest in the physiologic rest posture and/or when there is a tongue thrust, a cascade of negative impacts can occur. Just as the controlled forces of orthodontic appliances can move teeth, the abnormal functions and postures related to myofunctional disorders can influence the development of dental malocclusion, affect the position of the teeth, contribute to an improper bite relationship between the teeth in the upper and lower arches, cause a malformation of the bone of the dental arches, negatively influence the development of the facial structure, affect speech articulation, contribute to sleep-related breathing disorders, and affect general health and well-being.
WHAT IS A MYOFUNCTIONAL DISORDER?
Oral and Dental Development…
Abnormal pressures from the tongue on the teeth, parafunctional habits, clenching/grinding, tongue tie, and anything that disrupts the correct rest posture of the tongue/lips/jaws will likely affect tooth position, dental development, palate shape, development of the nasal cavity, proper breathing and oxygen intake, sleep breathing, and quality of life. Importantly, parafunctional habits and sucking habits such as thumb sucking, pacifier use, sippy cup use, nail biting (to name a few), can adversely affect the development of the mouth. A majority of the patients we see have a tongue thrust or a tongue/mouth rest position that has already adversely impacted their dental development. We see many orthodontic patients pre, during, and post orthodontics to help “get their tongue under control” so the braces/appliances can work and the effects maintain when the appliances are removed. Often times, we see patients who have a tongue thrust or improper rest posture of the tongue, and their teeth have relapsed after orthodontics or jaw surgery because they were not treated for their myofunctional issues.
Sleep Disordered Breathing, Snoring, and Sleep Apnea…
Humans are the only creatures on the planet in which the tongue is connected into the airway. This means that our tongue has the ability to fall back into our airway when sleeping which can disrupt breathing and oxygen intake. When the tongue does not maintain its correct resting posture (on the roof of the mouth) with the lips closed when a person is sleeping, that person is susceptible to snoring, apnea, and sleep breathing issues. When a person snores, has sleep apnea, or any sleep breathing issue in which the tongue blocks the airway, that can cause a reduction of oxygen intake throughout the night and may stop a person from entering deeper sleep cycles which are necessary for adequate health and functioning. The adrenaline released when a person with sleep apnea wakes up to gasp for air also has negative implications on blood pressure and the heart. Sleep breathing disorders affect a person’s health, mood, growth, development, quality of life, and can place that person at risk for serious life threatening conditions. A recent study revealed that approximately 10% of children have sleep-disordered breathing, 2-4% of the pediatric population has obstructive sleep apnea, and 80% of men and 90% of women have sleep-disordered breathing issues that remain undiagnosed. Interestingly, in a study in the journal of Pediatrics in 2009, 50% of children diagnosed with ADHD no longer met that diagnosis once their tonsils and adenoids were removed. This is because large tonsils and adenoids can cause sleep breathing disorders which will prevent a child from achieving a deep enough level of sleep to release adequate amounts of growth hormone to ensure proper growth and development of the nervous system as well as ideal behavioral functioning. When a child is sleep deprived, that child will usually become hyperactive in order to keep him/herself awake. A recent study that follow 11,000 children from infancy through the age of 7 years, the largest study on sleep-disordered breathing in children to date, revealed a strong and persistent connection between sleep-disordered breathing symptoms and in early life and behavior. The researchers indicated that children whose sleep-disordered breathing peaked at 6 or 18 months of age were between 40% and 100% more likely to develop behavioral problems by age 7 when compared to children who breathe normally during sleep. This research is the strongest evidence to date that snoring, mouth breathing, and apnea can have serious behavioral and social-emotional consequences for children. The findings also provide evidence that early childhood sleep-disordered breathing effects may only become apparent years later.
Speech Articulation and Myofunctional Disorders…
81% of children with speech articulation issues also have myofunctional issues, and if the myofunctional issue is not treated, the speech articulation challenge may never fully resolve.
WHAT ARE THE BENEFITS OF THE PHYSIOLOGIC REST POSTURE?
- a) The proper resting position of the tongue helps support the upper dental arch/palate, helps determine its width, and helps to allow the teeth to grow in properly. If the tongue tests and functions low, the palate has the opportunity to narrow which also means that that nasal cavity will be smaller. Nasal breathing can then become challenging and less effective.
- b) Breathing through the nose (as opposed to the mouth) helps the body fight germs, allergens, and allows the body to process up to 25% more oxygen. The nasal turbinates help to moisten, filer, and warm the air that we breathe in. Importantly, recent reserach has indicated that the nasal turbinates also release nitric oxide which fights pathogens and also allows the body to breakdown and process oxygen better. This is powerful information supporting how important it is to breathe through the nose and correct any mouth breathing patterns.
- c) The resting position of the tongue and jaws plays an important role in determining the shape and development of the facial structure.
- d) A tongue that does not have adequate resting tone may fall into the airway when a person is sleeping and will therefore contribute to sleep-breathing disorders such as snoring and sleep apnea. When a person snores, has sleep apnea, or any sleep breathing issues, his/her body receives less oxygen during sleep. Also, a level of deep sleep may not be reached, or may be less in duration. 90% of growth hormone is released when a person achieves a level of deep sleep, and a person may not release enough growth hormone to grow to his/her greatest potential if there is a sleep-related breathing issue. In many cases, the body also releases adrenaline to wake the person up from an apnea (low oxygen) incident during sleep. All of these above factors will likely have significant and serious life effects on health, mood, and growth/development for children and adults.
In sum, the benefits of the physiologic rest posture cannot be understated and also includes the following:
- Lip closure aids in the development of the muscles in the lower third of the face.
- Comfortable lip closure looks attractive.
- Lip closure helps keep the lips from drying out.
- Lip closure helps keep the mouth moist with saliva which has many benefits: saliva provides a defensive barrier against bacteria, fungi and viruses; it has a buffering action which protects teeth against bacteria producing acids; and there is a remineralizing benefit that helps repair the early stages of tooth decay.
- Lip closure helps eliminate or reduce bad breath.
- The lip and cheek muscles form a band that circles the teeth which determines the dimensions of the arch and establishes the position of the teeth.
- Lip closure helps to guide the anterior teeth into position and acts as a retainer to hold them in place.
- Lip closure establishes nasal breathing while awake and sleeping.
- Nasal breathing increases the lung’s ability to absorb oxygen from the inspired air.
- Diaphragmatic breathing, as part of the physiologic rest posture, pulls air into the lowest part of the lungs where oxygen exchange is most efficient.
- Diaphragmatic breathing lowers the heart rate and blood pressure, relaxes muscles, calms the mind and stops anxiety.
- Nasal breathing filters the air of debris and pathogens.
- Nasal breathing helps to shrink the nasal turbinates.
- Nasal breathing contributes to the normal development of the nasal cavity and the maxillary sinuses.
- Nasal breathing while sleeping helps reduce the dry or sore throat associated with mouth breathing.
- Nasal breathing produces a pattern of airflow which helps to suck the tongue up in the palate.The proper posture of the tongue in the palate is known as the neutral position.
- The neutral position aids in the normal development of the palate.
- The neutral position helps to support the palatal transverse arch width.
- The neutral position helps to maintain an open pharyngeal airway.
- The neutral position brings the tongue up off the floor of the mouth to facilitate free flow of the sub-lingual salivary glands.
- The neutral position helps support the mandible allowing the teeth to separate in freeway space.
- The physiologic rest posture with freeway space helps to relax the masseter muscles.
- The physiologic rest posture with freeway helps keep the temporomandibular joint ‘loose packed’ to maintain the proper disc space width.
- The physiologic rest posture with freeway space stops clenching or grinding while awake or sleeping.
- The physiologic rest posture helps to maintain proper head posture.
- The physiologic rest posture is the starting point for the correct saliva swallowing.
WHAT ARE THE BENEFITS OF CORRECT SALIVA SWALLOWING?
- Lip closure during the process of swallowing saliva seals the oral cavity so that the tongue can create the proper suction to move the saliva to the back of the mouth to be swallowed.
- During the process of sucking and swallowing the saliva, specific intrinsic and extrinsic muscles in the tongue contract which helps to reinforce the correct shape and position of the tongue.
- Proper muscle tonicity in the intrinsic and extrinsic tongue muscles helps to maintain the tongue in the neutral position.
- Normal sucking and swallowing of saliva with the tongue in the neutral position puts the pressure of the tongue in the palate not on the teeth which is extremely important because teeth are susceptible to the guidance and influence of pressure and stimulus.
- When the teeth come together or intercuspate during the saliva swallow, there is a stabilizing effect on the teeth by holding them in lateral or transverse and rotational relationship.
- The biting down during the swallow also prevents the extrusion or super eruption of the teeth which helps to maintain arch stability.
- Swallowing with the tongue in the neutral position causes the back of the tongue to lift up and close the airway preventing aspiration of the saliva.
- Proper swallowing with the tongue in the neutral position helps to open the Eustachian tubes to the middle ear.
- Correct saliva swallowing helps to correct drooling.
- Correct saliva swallowing helps to correct spitting during speech.
- Correct saliva swallowing helps to reinforce the correct swallowing pattern for liquids and food.
WHAT ARE THE BENEFITS OF CORRECT CHEWING AND SWALLOWING OF FOOD?
- Research indicates that we are to masticate during the process of eating 1000 to 3000 times per day; therefore it is important to use the lip, tongue and jaw muscles correctly.
- There are twenty pairs of muscles that are used during normal chewing and swallowing which helps to establish muscle balance between the two halves of the oral cavity.
- Lip closure during chewing and swallowing strengthens and develops the lip muscles which in turn helps establish lip closure for all the mouth functions.
- Lip closure during chewing and swallowing is proper etiquette.
- Lip closure prevents ‘smacking’ or noisy eating.
- Lip closure keeps food from spilling out or corrects the messy eater.
- Lip closure while chewing limits the side to side movement of the jaw which is beneficial for the temporomandibular joint.
- Thorough chewing dissolves substances in the food to make them more accessible to the taste buds.
- Chewing a semi-hard to hard diet in a child helps to develop the mandible.
- Proper bilateral chewing help to develop the two sides of the mandible evenly.
- Proper bilateral chewing promotes bilateral muscle development in the temporomandibular joints.
- Proper bilateral chewing helps distribute the force used by the chewing muscles evenly between both sides.
- Proper bilateral chewing helps produce a more uniform wear pattern on the teeth.
- Proper bilateral chewing contributes to facial symmetry.
- Proper tongue sweeping while chewing cleans debris off the teeth prior to the swallow.
- During the swallowing of food the pressure of the tongue is in the neutral position on the palate not against the teeth.
- The teeth intercuspate during the swallowing of the food helping maintain occlusal stability.
- Chewing correctly has many health benefits.
- Proper tongue function while chewing prevents premature entry of food into the throat which prevents choking.
- Thorough chewing increases saliva production which helps to digest bacteria that can lead to plaque buildup.
- Proper chewing thoroughly mixes the food with saliva which is rich in digestive enzymes that begin the process of starch and fat digestion.
- The more chewing, the more food is exposed to the anti-bacterial enzyme in the saliva that kills food-borne pathogens.
- When food is chewed thoroughly the less work there is for the stomach and intestines reducing gas and bloating.
- The intestines will have an easier time pulling micronutrients out of thoroughly chewed food.
- Thorough chewing provides the body with more vitamins, minerals, antioxidants and amino acids.
- Proper swallowing of food eliminates the swallowing of air reducing gas and belching.
- Chewing releases serotonin, a neurotransmitter that helps us relax, go to sleep, focus or concentrate and elevates our mood.
WHAT ARE THE BENEFITS OF NORMAL LIQUID SWALLOWS?
- Proper swallowing of liquids with the tongue in the neutral position allows the back of the tongue to lift up to close the airway to prevent aspiration of liquid into the lungs.
- The pressure of the tongue during the liquid swallow is in the palate not on the teeth.
- Normal swallowing of liquids eliminates the swallowing of air, reducing gas and belching.
- Normal swallowing of liquids eliminates ‘dribbling’.
- Normal swallowing of liquids stops ‘noisy’ drinking.
WHAT ARE THE BENEFITS OF PROPER MUSCLE FUNCTION FOR SPEECH?
- All speech sounds except the /th/ sounds are based in the neutral position.
- Speaking within the neutral position keeps the tongue from putting incorrect pressure on or between the teeth.
- Proper muscle tone in the intrinsic and extrinsic tongue muscles helps the tongue to move quickly and accurately to produce the various consonant sounds.
- Proper lip development aids in the production of the labial speech sounds.
- Normal jaw function during speech is produced within a ‘graded opening’ which does not stress the temporomandibular joint.
- Correct muscle function for speech can affect a person’s speech articulation, ability to be understood, and can also have positive social impacts.
WHAT CAUSES MYOFUNCTIONAL DISORDERS?
- Improper oral habits: such as thumb or finger sucking, prolonged pacifier use, sippy-cup use, cheek biting, lip licking, nail biting, bruxism (clenching/grinding)
- Restricted nasal airway due to enlarged tonsils/adeniods, allergies, sinusitis or a deviated septum, or any airway issue promoting an open mouth posture and/or mouth breathing.
- Structural or functional abnormalities such as a restricted lingual frenum (tongue-tie), narrow palate, or a short upper lip
- Neurological or developmental abnormalities.
- Hereditary predisposition to some of the above factors
The mouth, also known as the oral cavity, is a complex organ composed of three systems: the myofunctional system, the dental system and the medical system. There is no one specific cause for myofunctional disorders. There may be multiple contributing or causative factors within these three systems that negatively influence how the 5 basic mouth functions will work.
MYOFUNCTIONAL SYSTEM:
The following are conditions within this myofunctional system make it difficult for the orofacial muscles to function correctly.
LIPS: There are different conditions that affect the function of the lips:
- Short upper lip
- Restricted maxillary frenum (skin between the upper lip and gums)
- Everted lower lip
- Flaccid orbicularis oris muscle
- Tight mentalis muscle
- Tight platysma muscle
TONGUE: There are different conditions that affect the function of the tongue:
- Incorrect development of the intrinsic and extrinsic tongue muscles
- Restricted lingual frenum (skin under the tongue)
- Enlarged tonsils
- Restricted palate
JAW: There are different conditions that affect the function of the jaw:
- Jaw muscle pain, injury, nerve damage, etc.
- Disc displacement
- Dental discrepancies
DENTAL SYSTEM:
Conditions within the dental system can make it difficult for the orofacial muscles to function correctly.
- Shape of the hard palate
- Relationship between the upper and lower arches
- Alignment of the teeth
- Dental appliances on the palate, on the teeth or between the teeth
MEDICAL SYSTEM:
Conditions within the medical system can make it difficult for the orofacial muscles to function correctly.
- Restricted nasal airway
- Enlarged tonsils or adenoids
- Allergies, asthma, respiratory problems, etc.
- Syndromes, neurological conditions, injury, etc.
All of these systems and structures work together as a team. A dysfunction or altered functional pattern in any one of them affects the others, contributing to myofunctional disorders.
WHAT CAUSES TONGUE THRUST?
- Improper oral habits: such as prolonged thumb or finger sucking, cheek/nail biting, tooth clenching/grinding.
- Restricted nasal airway: due to enlarged tonsils/adeniods, allergies, sinusitis or a deviated septum, which promotes habitual open-lip posture.
- Structural or functional abnormalities such as a short linqual frenum (tongue-tie).
- Neurological or developmental abnormalities.
- Hereditary predisposition to some of the above factors
- Improper oral habits: such as thumb or finger sucking, prolonged pacifier use, sippy-cup use, cheek biting, lip licking, nail biting, bruxism (clenching/grinding)
- Restricted nasal airway due to enlarged tonsils/adeniods, allergies, sinusitis or a deviated septum, or any airway issue promoting an open mouth posture and/or mouth breathing.
- Structural or functional abnormalities such as a restricted lingual frenum (tongue-tie), narrow palate, or a short upper lip
- Neurological or developmental abnormalities.
- Hereditary predisposition to some of the above factors
The mouth, also known as the oral cavity, is a complex organ composed of three systems: the myofunctional system, the dental system and the medical system. There is no one specific cause for myofunctional disorders. There may be multiple contributing or causative factors within these three systems that negatively influence how the 5 basic mouth functions will work.
MYOFUNCTIONAL SYSTEM:
The following are conditions within this myofunctional system make it difficult for the orofacial muscles to function correctly.
LIPS: There are different conditions that affect the function of the lips:
- Short upper lip
- Restricted maxillary frenum (skin between the upper lip and gums)
- Everted lower lip
- Flaccid orbicularis oris muscle
- Tight mentalis muscle
- Tight platysma muscle
TONGUE: There are different conditions that affect the function of the tongue:
- Incorrect development of the intrinsic and extrinsic tongue muscles
- Restricted lingual frenum (skin under the tongue)
- Enlarged tonsils
- Restricted palate
JAW: There are different conditions that affect the function of the jaw:
- Jaw muscle pain, injury, nerve damage, etc.
- Disc displacement
- Dental discrepancies
DENTAL SYSTEM:
Conditions within the dental system can make it difficult for the orofacial muscles to function correctly.
- Shape of the hard palate
- Relationship between the upper and lower arches
- Alignment of the teeth
- Dental appliances on the palate, on the teeth or between the teeth
MEDICAL SYSTEM:
Conditions within the medical system can make it difficult for the orofacial muscles to function correctly.
- Restricted nasal airway
- Enlarged tonsils or adenoids
- Allergies, asthma, respiratory problems, etc.
- Syndromes, neurological conditions, injury, etc.
All of these systems and structures work together as a team. A dysfunction or altered functional pattern in any one of them affects the others, contributing to myofunctional disorders.
WHO MIGHT REFER FOR MYOFUNCTIONAL THERAPY?
- Dental specialists
- Medical specialists
- TMJ specialists
- Osteopath
- Chiropractor
- Physical therapist
- Speech pathologist
- Occupational therapist
WHAT CONDITIONS ARE REFERRED FOR MYOFUNCTIONAL THERAPY?
- Sucking habits
- Parafunctional habits
- Mouth breathing
- Lip incompetence-the inability to close the lips without muscle strain
- Drooling
- Chapped lips
- Red swollen gums; excess plaque
- Incorrect tongue posture at rest
- Sleep disordered breathing
- Bruxism-clenching or grinding the teeth in other than normal function
- Jaw muscle pain
- Cracking or fracturing teeth
- Tongue thrust-the incorrect action of the tongue while swallowing saliva, chewing and swallowing food, liquid swallows and/or during speech
- Incorrect relationship between the upper and lower arches
- Malocclusion
- Orthodontic/orthognathic surgical relapse
- Eating dysfunction
- Choking or aspirating
- Lazy speech muscles
Any one or a number of specialists may recognize a problem in a child, adolescent or adult and want the patient to go through myofunctional therapy.
HOW DOES MYOFUNCTIONAL THERAPY WORK?
DISCIPLINE is defined as training of the physical powers by exercises, instructions and control.
- EXERCISES tone the muscles, changing their shape, strength, range of motion and their ability to coordinate with other muscles.
- INSTRUCTIONS develop consistent production of the correct functions.
- CONTROL of the new functions through self-monitoring and
self-correction in order to habituate the correct functions.
TIME is an essential element in the process of rehabilitating the orofacial muscles and the functions.
- It will take time to tone the muscles with the exercises.
- It will take time to retrain the muscles to function correctly through the instructions.
- It will take time to control the correct muscle functions in order to form new habits.
The principles of myofunctional therapy are the same for children, adolescents or adults: exercises, instructions on normal function and learning to control the new function.
WHY SHOULD YOU BE CONCERNED?
- Dental Development: Orthodontists have been concerned about myofunctional disorders since the early 1900’s because the abnormal functions and postures of myofunctional disorders can adversely influence dental growth, slow orthodontic treatment and can undermine the stability of the correction which can cause the teeth to relapse after orthodontics. Just as orthodontic appliances such as braces can move teeth, the abnormal pressures from the tongue will adversely influence the development of the mouth
- Speech Articulation: Research has revealed a high incidence of speech problems in those individuals who exhibit myofunctional disorders. The /s/ sound is the most common, others are /z/,/sh/, /ch/,/j/, /t/, /n/ and /r/. 81% of children with speech articulation issues also have myofunctional issues, and if the myofunctional issue is not treated, the speech articulation challenge may never fully resolve.
- Eating and Digestion: Individuals who exhibit myofunctional disorders frequently have poor chewing/eating functions such as being noisy and messy eaters, swallowing food without fully chewing it, and chewing food with their lips open. All this can have a negative impact on digestion.
- TMJ Dysfunction and Facial Pain: The temporomandibular joint (TMJ) may be negatively affected when a myofunctional disorder is present, thus causing facial pain and other oral-facial problems.
- Sleep Breathing: Snoring, sleep apnea, and sleep-breathing issues co-occur with myofunctional disorders when the lips and tongue do not function in the correct position when sleeping. Sleep-breathing disorders often affect a person’s health, mood, growth/development, quality of life, and can place that person at risk for serious life-threatening conditions.
- General Health: A habitual open mouth posture and mouth breathing can lead to an increased incidence of chronic sore throats, upper respiratory illness, allergies, and other breathing issues. Establishing correct nasal breathing pattern and tongue posture can lead to a lifetime of better health.
HOW EFFECTIVE IS MYOFUNCTIONAL THERAPY?
WHAT DOES PROGRESS IN MYOFUNCTIONAL THERAPY DEPEND ON?
- The number of myofunctional problems that need to be corrected as determined with a diagnostic myofunctional evaluation.
- Any medical condition/s that would compromise the goals of therapy.
- Dental conditions affecting the palate or teeth that make it difficult for the muscles to function correctly.
- Patient compliance with the myofunctional therapy exercises and the daily practice to retrain the muscles to function correctly.
- Parental involvement with young patients to supervise the exercises and give guidance on proper function.
- Keeping the therapy appointments.
- The frequency of interruptions in the routine of doing the exercises or practicing the proper functions, i.e. holidays, vacation, illness, school issues, work situations, etc.
- Controlling any parafunctional habit, action or behavior that works against the goals of therapy.
IS MYOFUNCTIONAL THERAPY FOR CHILDREN DIFFERENT THAN FOR ADULTS?
Children do present more challenges in the rehabilitation process due to the following that include, but are not limited to:
- Sucking habits (digits, pacifier, clothes, toys, etc.)
- Parafunctional habits (i.e. nail biting, excessive licking, gum chewing, sipper cups or bottles, straws, etc.)
- Medical airway conditions (colds, sore throats, tonsillitis, allergies, etc.)
- Dental conditions (loose teeth, sore mouth, appliances, etc.)
- Age
- Motivation (20% of all children are self-motivated, 60% are other motivated and 20% are not motivated)
- Patient cooperation
- Parental involvement
- Extracurricular activities
- After school care
- Frequency of school holidays which interferes with the routine of therapy
Regardless of all the challenges involved in doing therapy with children, when myofunctional problems are noted therapy should be started immediately to correct the lack of proper muscle development and improper oral function.
IF THERAPY FOR CHILDREN PRESENTS MORE CHALLENGES, WHY NOT JUST WAIT UNTIL THEY ARE OLDER TO BEGIN THERAPY?
- The first reason involves ontogeny. Ontogeny is the process through which a system grows and develops to perform specialized functions. The ontogeny of the oral cavity begins at birth and reaches maturity around 18 to 25 years of age. Ontogeny includes both genetics and function. According to research, 90% of babies are born genetically perfect; but the greatest stimulus to continued proper development comes from the correct functional patterns.
It is important to note that from birth to age four there is a large increase in the development of the oral cavity including the acquisition of the primary teeth and the development of the five basic mouth functions. Then from age four to age twelve 90% of the development of the oral cavity is reaching maturity.
- The second reason for early intervention is that myofunctional problems tend to be progressive. If disorders in young children are not treated, the implication is that delaying treatment can result in a greater more complex problem; require more extensive, more complicated or more expensive solutions; with a possibility that delayed treatment results will not be as good as what could be achieved with early intervention.
Taking all these factors into consideration, the child will be given therapy that is age appropriate. If they are not able to comply with therapy exercises and instructions, the focus would be on eliminating any parafunctional habits that compromise the oral cavity then resume myofunctional therapy at a later date.
In children, high levels of normal function must be maintained through the process of ontogeny to stimulate the highest growth and development of the oral cavity structures, muscles and functions.
WHAT CAN I DO TO HELP MY CHILD DEVELOP NORMAL FUNCTION TO TRY TO AVOID FUTURE PROBLEMS?
Here is the information I gave him, which he and his wife implemented as soon as their daughter Talia was born because normal function begins at birth.
NURSE
- Nurse for a minimum of 6 months to 1 year or longer if possible to help with normal muscle development and function.
- Nursing at the breast is the physiologic catalyst that sets up the specialized functions of normal nasal breathing, normal tongue posture, and normal swallowing patterns that we want children to use through the process of ontogeny and into adulthood.
- If there are problems nursing, check with a lactation specialist to determine if the lingual frenum or the maxillary labial frenum is restricted, making it difficult for the infant to latch on or seal their lips properly to create the proper sucking function.
- If nursing is not possible, use the smallest bottle nipple possible to encourage vigorous sucking then eliminate the bottle by age 1 year.
- When a child nurses, the breast nipple conforms to the oral cavity but when a foreign object goes in the mouth, the oral cavity adapts to the foreign object.
- Nursing not only helps with the normal growth and development of the oral cavity, it is also the primary source of pacification.
PACIFICATION
- If an infant needs additional pacification and will accept a pacifier, use the smallest pacifier nipple possible to simulate proper tongue and lip muscle function.
- A newborn cannot self-soothe and relies on sucking as a primary source of pacification. Sucking releases serotonin, a neurotransmitter that helps us fall asleep and stay asleep, calms us, elevates our mood and helps us focus or concentrate.
- Around age 4 to 6 months a baby begins to roll over and wiggle his/her arms and legs, releasing serotonin, which helps to pacify the child. They can now self-soothe, and any sucking habit whether a pacifier, digit, blanket, or toy, etc. should be eliminated.
DRINKING
- Babies begin to show an interest in drinking from a cup at around age 6 months.
- All drinking from this point forward should not be a sucking action but should be free flow drinking to help the lip and cheek muscles develop correctly.
- The lip and cheek muscles form a band that circles the teeth which determines the position of the teeth and the dimension of the dental arches.
- Normal cheek muscle pressure is 2 grams/per square centimeter to allow for the normal expansion of the dental arches which is influenced by genetics and the function of the tongue in the palate.
- The use of a straw, a sippy cup, pacifier, digit or bottle is a sucking action. This sucking action is like sending the cheek muscles to the gym and working them out. The cheek muscle pressure can increase to 20 grams in the molar region and 80 grams in the cuspid region resulting in narrowing of the dental arches.
- If you are concerned with spilling, use a cup with a small opening like the Playtex Coolster Tumbler and remove the valve so it is not a sucking cup but a free-flow drinking cup. The small opening will minimize spilling. There are also other spill-proof cups with lids that can be used, just ensure that the child is not required to suck in order to get the liquid out.
EATING
- Encourage the child to chew with his/her lips closed.
- Chew small to moderate sized bites.
- Encourage the use of child-sized utensils to control bite size.
- Chew on both sides of the mouth.
- Chew and swallow the bite before putting more food in.
- By age 4, the child should be able to chew a semi-hard to hard diet.
- Do not use the sucking pouches that contain pureed fruits and vegetables, this is a sucking action and works the cheek muscles.
PARAFUNCTIONAL HABITS
- All oral habits that fall outside the 5 basic mouth functions should be eliminated.
- Eliminate all sucking habits, thumb, fingers, arm, hand, blanket, toys, clothes, etc. If you need assistance a Certified Orofacial Myologist is trained to help families eliminate sucking habits.
- No excessive licking; biting nails or stuff; no chewing gum, etc.
- No mouth breathing except for physical activity or nasal congestion. If nasal congestion is suspected, consult your pediatrician or Ear, Nose and Throat specialist.
LA JOLLA / TORREY PINES
SDCST
3535 General Atomics Ct.
San Diego, CA 92121
(Inside the Nautilus Three Building, where Water & Sports PT is located)
3535 General Atomics Ct.
San Diego, CA 92121
(Inside the Nautilus Three Building, where Water and Sports PT is located)
CORONADO
SDCST
120 C Avenue Unit 110
Coronado, CA 92118
(located inside Water and Sports PT)
120 C Avenue Unit 110
Coronado, CA 92118
(Located inside Water & Sports Physical Therapy)